Published July 13, 2017
PORTLAND, Ore. – Last summer, Dwight Holton was fed up. The CEO of Lines for Life, which runs Oregon’s drug and alcohol health line and suicide crisis line, worked for years to get the state’s doctors to prescribe fewer opioids.
“I have been working on this issue since 2010,” he said. “I thought I had been very patient. I started to move from patient to pissed off.”
Holton watched year after year as doctors across the state kept issuing bountiful prescriptions for addictive opioids such as hydrocodone and oxycodone. He said since the 1990s, drug companies have touted opioids as a high-reward, low-risk option for chronic pain, while the opposite was true. That sent the state, and states across the country, into a daunting opioid epidemic. Hospitalizations and deaths from opioids rose, and people struggling with chronic pain added addiction to their lists of ailments.
But then Holton received surprisingly good news: In 2015, opioid prescriptions dropped in nearly all Oregon counties.
Newly released data from the Centers for Disease Control shows doctors are prescribing fewer opioids in 28 out of 36 counties in Oregon. Many counties saw the numbers drop by a third to half.
But that doesn’t mean the problem is going away anytime soon. About 280 million opioid pills were prescribed in Oregon last year.
The issue persists the most in rural parts of the state. Oregonians in rural counties are far more likely to be prescribed opioids and with higher unemployment rates, lower incomes and less access to treatment centers, those who become addicted have more difficulty fighting back.
The data
The CDC released a report in July that showed opioid prescriptions decreased across the country, from about 782 morphine milligram equivalents per person in 2010 to 640 MME in 2015.
The CDC measures prescriptions in MME, which can translate across varying strengths of opioids. Hydrocodone is a one-to-one ratio: One milligram of hydrocodone is one MME.
Stronger opioids, like oxycodone and methadone, are higher than a one-to-one ratio – two tablets of 15 mg oxycodone is equal to 50 MME, and three tablets of 5 mg methadone is 50 MME.
A common prescription tablet of 5 mg hydrocodone is five MME. That means in 2010, the average American was prescribed about 156 tablets of 5 mg hydrocodone. In 2015, that dropped to 128 tablets per person.
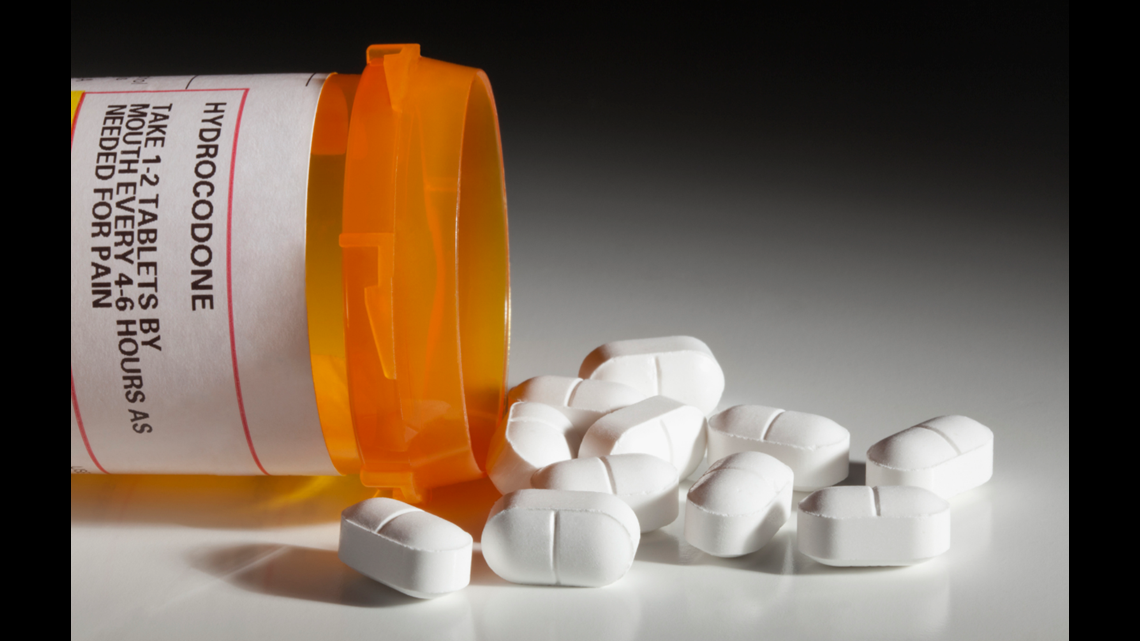
Oregon saw a drop from an average of 1186 MME per capita in 2010 to 972 in 2015 – or 237 five-milligram hydrocodone tablets to 194 tablets per person.
That drop was not consistent across the state. Oregon’s urban counties, such as Multnomah, Clackamas and Washington, had far lower prescribing rates than most rural counties.
The counties with the most opioids prescribed were in rural, isolated parts of the state, as were counties that saw their prescription numbers rise or remain stagnant.
Morrow, Wallowa, Malheur and Union counties all had more opioid prescriptions in 2015 than in 2010. Baker, Umatilla, Crook and Jefferson counties all saw their numbers stay about the same.
The worst county for prescriptions is in deep southern Oregon.
Rural Oregon struggles to combat opioid issues
Sunny Curry County borders California and is home to some of Oregon’s most beautiful beaches. It also has the highest number of opioid prescriptions in the state. Doctors prescribed 1800 MMEs per person in Curry County, on average, in 2015. That’s a drop from a staggering 2197 MMEs in 2010.
Curry County’s prescription numbers aren’t just high for Oregon. It’s the 74th worst county in the U.S. for opioid prescriptions.
Opioids aren’t the only drugs doctors are prescribing, either. State data shows Curry County has the highest rate of benzodiazepine prescriptions, with 133 prescription fills per 1,000 residents in the first three months of 2017. Curry County is also second in muscle relaxant prescriptions, methadone prescriptions and fourth in non-benzodiazepine sedative prescriptions in the state.
Residents of Curry County struggle with high unemployment rates – 8.6 percent as of 2015 – and relatively low income, at $35,720 per person based on 2014 data, which is the latest available.
It also has a host of other factors that triggered the Oregon secretary of state’s office in 2016 to identify it as a high-risk county. A review noted many county services, including health and human services, have transitioned to nonprofit agencies.
Holton notes rural counties often have less access to treatment centers and alternative pain management therapies, so doctors may prescribe at higher rates because fewer options are available.
But some Oregon counties that also have high unemployment rates and low incomes saw a dramatic drop in opioid prescriptions. Grant County, which has the state’s highest unemployment rate in 2015 at 9 percent, dropped from 882 MMEs per capita in 2010 to just 39 in 2015.
“All of our providers are very cautious in their opiate prescribing practices,” said Jessica Winegar, manager of the Grant County Health Department. She noted that Grant County, like much of the state, has readily adopted state and federal guidelines that caution against chronic opioid use and advocate for alternative pain therapies.
Winegar also said the availability of medical marijuana could have impacted opioid prescriptions, too.
“The increased availability of marijuana might help some people who choose to use it instead of opiates for their chronic pain and/or addiction issues,” she said.
But Winnegar noted Grant County continues to commonly see opiate-addicted patients.
The CDC said the prescription data is based on the pharmacies where prescriptions are filled. In Grant County, which has few pharmacies, residents may have traveled to other counties, such as Baker, to fill prescriptions.
How the state is fighting back
Opioid addiction can happen quickly and unintentionally, especially among patients prescribed opioids for chronic pain. Holton said someone who is prescribed opioids for 30 days has a 47 percent chance of still being on those prescribed drugs three years later. People who have a 90-day prescription have a 60 percent chance of being on opioids five years later.
The CDC has issued stern guidelines for opioid prescriptions in response to the country’s opioid epidemic. No longer are opioids a go-to pain resource. Instead, they urge limited prescriptions and encourage doctors to steer patients toward alternative therapies such as physical therapy.
The Oregon Health Authority has developed a robust set of recommendations for doctors who would have otherwise prescribed opioids for pain.
“OHA, with our local and state partners, have developed a four-pronged approach aimed at improving pain treatment for patients, including encouraging non-opioid pain management methods, and improving best practices for acute and palliative care; reducing harms to patients by ensuring medication-assisted treatment is available for opioid use disorder, and making naloxone rescue medication available; reducing the amount of opioids in the community through the establishment of prescribing guidelines, and encouraging safe storage and disposal of opioid medication; and using data to target and evaluation our interventions,” said OHA spokesman Jonathan Modie.
Modie noted the approach seems to be working. Prescriptions are down, as are overdose hospitalizations and deaths.
That’s especially good news for Oregon’s older adult population. Despite perceptions, the people suffering the most from opioid addiction in Oregon are seniors and adults age 45-64. Seniors and women have the highest rates of opioid-related hospital stays, according to the Agency for Healthcare Research and Quality and the Healthcare Cost and Utilization Project. In many rural counties such as Curry County, adults age 45-64 had the highest rates of hospitalization from opioids.
The fight against opioid addiction is a war with a key battle fought in doctor’s offices. The fewer opioids prescribed, the fewer pills infiltrate the community and fewer Oregonians gain access to highly addictive drugs.
But another battle is harder to crack down on. The Oregon Health Authority notes the CDC data doesn’t include illicit opioid use.
“We also have one of the highest rates of non-medical use of opioids, especially by young adults,” Modie said.
Heroin has long been the street opioid of choice but its stronger cousin, fentanyl, and ultra-potent carfentanil are emerging as extremely dangerous alternatives. There’s also no lab testing street drugs. Instances of overdose and death from black-market opioids are rising across the country.
State leaders say it’s a matter of time before these drugs take a toll on Oregon.
“On the horizon, we have synthetic fentanyl that is devastating eastern states,” Holton said. “It hasn’t gotten here in force yet but we’re all bracing for it.”
Interactive graphic by Jeff Patterson
Published July 13, 2017